Pancreatic Cancer
Pancreatic Cancer is cancer which starts in the organ behind the lower part of the stomach (pancreas – gland located deep in the abdomen, between the stomach and the spine). It begins when abnormal cells in the pancreas grow and divide out of control and form a tumor. It helps to makes enzymes for digestion and hormones which could control blood sugar levels.
Some organs are made up of cells, so does pancreas. Cells divide to form new cells as per the body’s requirement. Usually, old cells died and a new cell takes the place. But sometimes the process breaks. New cells form or old cells do not die, even if the body does not need them. The extra cell may form a mass of tissue which is known as a tumor.
Few tumors are mild which means they are unnatural but cannot penetrate other parts of the body. A destructive tumor is called cancer. The cells develop out of control and can expand to other tissues and organs.
Even if cancer expands to other areas of the body, it is still called pancreatic cancer if that is where it started. It often spreads to the liver, abdominal wall, lungs, bones and/or lymph nodes.
Types of Pancreatic Cancer
- Exocrine tumors: It is the most common type of pancreatic cancer. Adenocarcinoma is the most basic type of exocrine tumor. These tumors normally start in the tubes of the pancreas, called ductal adenocarcinoma. If the tumor arises in the acini, it is called acinar adenocarcinoma.
-
- Endocrine tumors: These are also known as pancreatic neuroendocrine tumors (PNETs) or islet cell tumors. They are not similar to exocrine tumors. A pancreatic neuroendocrine tumor functions a few times only. Only a functioning tumor makes hormones. A functioning neuroendocrine tumor is defined based on the hormone made by cells. They include: Insulinoma, Gastrinoma, Glucagonoma, Somatostatinoma, VIPomas, PPomas
Pancreatic Cancer Risk Factors
Factors which may raise a person’s risk of developing pancreatic cancer are following:
- Age (risk of developing pancreatic cancer increases with age)
- Gender (More females are affected rather than males)
- Smoking & Drinking (access amount may be the cause of a pancreatic cancer in early age)
- Obesity and diet (being overweight)
- Diabetes
- Family history (It’s less than one in 10%)
- Families with two or more first-degree relatives (parent, brother, sister or child) with pancreatic cancer
- Families with three or more relatives with pancreatic cancer on the same side of the family
- Families with a family cancer syndromeand at least one family member with pancreatic cancer. Family cancer syndromes are rare genetic conditions where a faulty gene increases the risk of pancreatic cancer.
- Rare inherited conditions.
- red and processed meat
- gallstones and gall bladder surgery
Book Appointment
Quick Contact
- Address 557A1/15C Gultekadi, Market Yard Pune, Maharashtra 411037
- Email social.prolife@gmail.com
- Phone +91-9607079019, +91-9607079029
What are the symptoms of Pancreatic Cancer?
In the majority of cases, symptoms develop after the growth of pancreatic cancer.
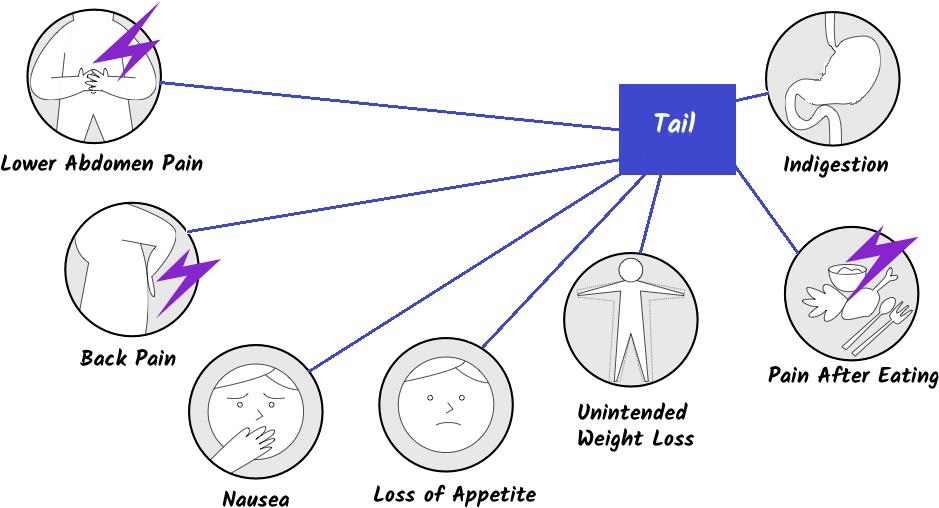
Signs of Pancreatic Cancer may include:
- Jaundice (yellow eyes, Light-colored or greasy stools, Dark urine, itchy skin)
- Belly(abdomen) pain or back pain
- Weight loss and poor appetite (bloating)
- Nausea and vomiting
- Gallbladder or liver enlargement
- Blood clots
- Diabetes
These signs usually do not mean you have Pancreatic cancer. But if you see one or more of them for more than two weeks, consult your doctor.
How can it be diagnosed?

Doctor may have you undergo the following tests if suspects pancreatic cancer
- Imaging tests: (creates pictures of your internal organs) These examinations assist your doctors to visualize your internal glands, including the pancreas. The methods used to diagnose pancreatic cancer are ultrasound, computerized tomography (CT) scans, magnetic resonance imaging (MRI) and, sometimes, positron emission tomography (PET) scans.
- Ultrasound: (Using a scope to create pictures of your pancreas) An endoscopic ultrasound (EUS) uses an ultrasound device to take pictures of your pancreas from inside your abdomen. The device is transferred through a thin, flexible tube (endoscope) down your esophagus and into your stomach to obtain the images.
- Biopsy: (Removing a tissue sample for testing) It is a method to extract a tiny sample of tissue for a test under a microscope. Your doctor may collect a sample of tissue from the pancreas by injecting a needle through your skin and into your pancreas (fine-needle aspiration). Or by removing a sample during EUS, guiding special tools into the pancreas.
- Blood test. The doctors test the blood for specific proteins (tumor markers) shed by pancreatic cancer cells. The market test used in One tumor marker in pancreatic cancer is called CA19-9. There is no guarantee of the test and it is not clear how best to use the CA19-9 test results. Some doctors rank your levels throughout the treatment.
If pancreatic cancer confirms after the diagnosis, then the Doctor determines the extent (stage) of cancer. Doctor assigns a stage of pancreatic cancer after the stage tests. It helps to decide the most likely treatments.
Stages of Pancreatic Cancer
Stage 0 or Carcinoma in situ:
The cancer is confined to the top layers of pancreatic duct cells and has not invaded deeper tissues. It has not spread outside of the pancreas. These tumors are sometimes referred to as carcinoma in situ (Tis). It has not spread to nearby lymph nodes (N0) or to distant sites (M0).
Stage I:
IA : The cancer is confined to the pancreas and is no bigger than 2 cm (0.8 inch) across (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0).
IB : The cancer is confined to the pancreas and is larger than 2 cm (0.8 inch) but no more than 4cm (1.6 inches) across (T2). It has not spread to nearby lymph nodes (N0) or to distant sites (M0).
Stage II:
IIA : The cancer is confined to the pancreas and is bigger than 4 cm (1.6 inches) across (T3). It has not spread to nearby lymph nodes (N0) or to distant sites (M0).
IIB : The cancer is confined to the pancreas and is no bigger than 2 cm (0.8 inch) across (T1) AND it has spread to no more than 3 nearby lymph nodes (N1). It has not spread to distant sites (M0).
The cancer is confined to the pancreas and is larger than 2 cm (0.8 inch) but no more than 4cm (1.6 inches) across (T2) AND it has spread to no more than 3 nearby lymph nodes (N1). It has not spread to distant sites (M0).
The cancer is confined to the pancreas and is bigger than 4 cm (1.6 inches) across (T3) AND it has spread to no more than 3 nearby lymph nodes (N1). It has not spread to distant sites (M0).
Stage III:
The cancer is confined to the pancreas and is no bigger than 2 cm (0.8 inch) across (T1) AND it has spread to 4 or more nearby lymph nodes (N2). It has not spread to distant sites (M0).
The cancer is confined to the pancreas and is larger than 2 cm (0.8 inch) but no more than 4cm (1.6 inches) across (T2) AND it has spread to 4 or more nearby lymph nodes (N2). It has not spread to distant sites (M0).
The cancer is confined to the pancreas and is bigger than 4 cm (1.6 inches) across (T3) AND it has spread to 4 or more nearby lymph nodes (N2). It has not spread to distant sites (M0).
The cancer is growing outside the pancreas and into nearby major blood vessels (T4). The cancer may or may not have spread to nearby lymph nodes (Any N). It has not spread to distant sites (M0).
Stage IV:
The cancer has spread to distant sites such as the liver, peritoneum (the lining of the abdominal cavity), lungs or bones (M1). It can be any size (Any T) and might or might not have spread to nearby lymph nodes (Any N).
What are the treatment options for Pancreatic Cancer?

- Surgery
- Whipple procedure: A surgical method in which the head of the pancreas, the gallbladder, part of the stomach, part of the small intestine, and the bile duct are removed. Enough of the pancreas is left to produce digestive juices and insulin.
- Total pancreatectomy: This surgery removes the whole pancreas, part of the stomach, part of the small intestine, the common bile duct, the gallbladder, the spleen, and nearby lymph nodes.
- Distal pancreatectomy: Operation to remove pancreas body and the tail. The spleen may also be removed if cancer has spread to the spleen.
- Biliary bypass: If cancer is obstructing the bile duct and bile is building up in the gallbladder, a biliary bypass may be done. During this operation, the doctor will cut the gallbladder or bile duct in the area before the blockage and sew it to the small intestine to create a new pathway around the blocked area.
- Endoscopic stent placement: If the tumor blocks the bile duct, an operation may be done to put in a stent (a thin tube) to drain bile that has built up in the area. The surgeon may place the stent through a catheter that drains the bile into a bag on the outside of the body or the stent may go around the blocked area and drain the bile into the small intestine.
- Gastric bypass: If the tumor blocks the flow of food from the stomach, the stomach may be sewn directly to the small intestine so the patient can continue to eat normally.
- Targeted therapy
- Radiation therapy
- External radiation therapy : A machine outside the body send a radiation toward cancer.
- Internal radiation therapy : radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near cancer.
- Diet
- Exercise
- Pain medicine
- Bowel movements
Follow-up appointments

After you’ve completed your treatments for Pancreatic cancer, follow-up care is very essential. Routine checkups can help find any changes in your health, and if cancer comes back (or “recurs”), it can be treated as soon as possible.
If your treatment has finished, follow-up appointments maybe every 3−6 months for the first couple of years and 6−12 months for the following 3 years.
Your doctor may check your CEA level before you begin treatment and again after treatment to understand if it has come down.
Doctors recommend CT scans of the chest, abdomen, and pelvis n a daily schedule for 3 years in people who are at high risk for recurrence.
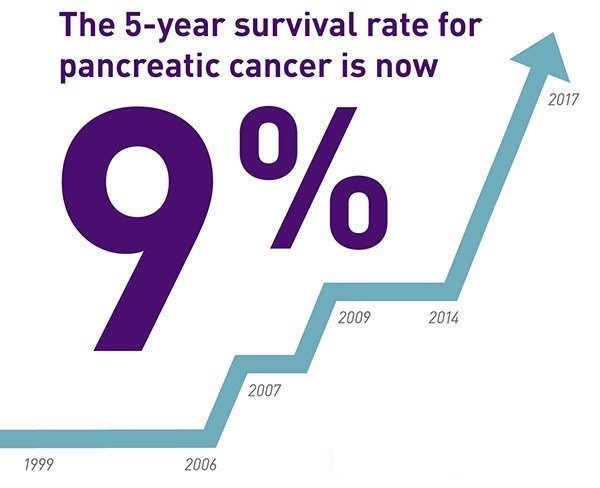
Pancreatic Cancer Statistics
The 5-year survival rate for people with stage 4 pancreatic cancer is nearly 1 percent. This means that 1 out of every 100 people with this type of cancer are still alive 5 years after their diagnosis. Any survival rate is an estimate. Some other researchers place the 5-year survival rate at 2 percent or 3 percent.
The risk for a person with cancer depends on many factors to a particular person
Why choose Prolife Cancer Centre for Your Pancreatic Cancer Care?

At Prolife Cancer Center, your Pancreatic cancer treatment is personalized to give the best results, while concentrating on your quality of life. We offer minimally invasive laparoscopic surgeries that provide successful treatment with less impact on you.
Specialized Pancreatic Cancer Treatments
Prolife offers unique options. Our globally renowned team of physicians shows your treatment for the most benefit while reducing the impact on your body.
Dr. Sumit Shah is expertise in treating Pancreatic cancer. We offer the best Laparoscopic surgery treatment for pancreatic cancer also chemotherapy and targeted therapy options.

